Elevate Gastroenterology Care with Specialized Billing Services
Expert Revenue Cycle Services for Your Digestive Health Practice
Home > Medical Specialties > Gastroenterology
Gastroenterology Billing Services
Gastroenterology billing services require specialized expertise due to complex diagnostic procedures, endoscopy coding requirements, and evolving payer reimbursement guidelines. MBW RCM demonstrates strong competence in gastroenterology billing and coding through accurate documentation review, compliant coding practices, and structured revenue cycle management workflows.
Gastroenterology focuses on diseases and disorders affecting the digestive system, including the gastrointestinal tract from the mouth to the anus. Billing for these services often involves advanced procedures such as colonoscopy, endoscopy, motility testing, and evaluation and management (E/M) services. Accurate billing requires precise documentation and correct application of CPT, ICD-10, and HCPCS codes.
MBW RCM applies specialty-focused billing expertise to manage these complexities and support efficient gastroenterology revenue cycle operations.
The Complexity of Gastroenterology Billing
Medical billing and coding in gastroenterology can be challenging due to the variety of diagnostic and therapeutic procedures performed within the specialty.
Several factors contribute to the complexity of gastroenterology billing, including:
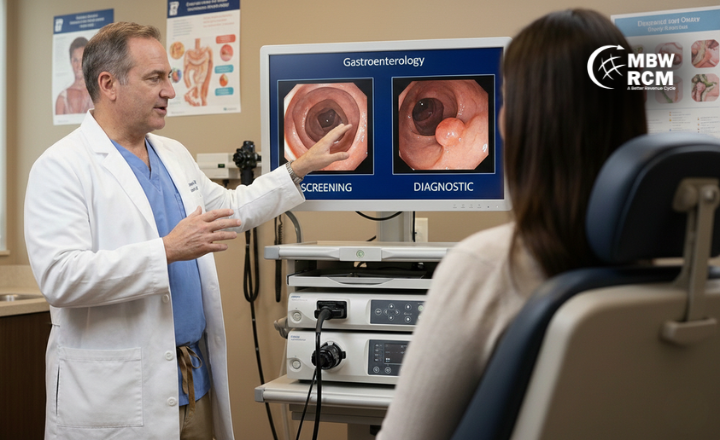
Differentiating colorectal cancer screening procedures from diagnostic colonoscopies
Billing for motility studies and gastrointestinal function tests
Documenting appropriate levels of evaluation and management services
Applying Category III CPT codes for emerging treatments such as GERD procedures
Correct use of modifiers such as -51, -59, and -26
Accurate coding and documentation are essential to ensure compliant billing and appropriate reimbursement for gastroenterology services.
Endoscopy Billing and Underpayment Tracking
Endoscopy procedures represent a significant portion of gastroenterology services and require precise coding and documentation. Billing accuracy depends on correctly documenting procedural details and identifying potential reimbursement discrepancies.
Underpayment tracking is particularly important in gastroenterology billing, as reimbursement differences can occur due to payer policies, coding errors, or incomplete documentation. Effective underpayment identification helps ensure that services are reimbursed according to payer contracts and coding guidelines.
MBW RCM’s Expertise in Gastroenterology Billing
MBW RCM’s billing and coding professionals maintain specialty expertise in gastroenterology revenue cycle management. Our teams support healthcare organizations across all 50 states, including hospitals, physician groups, and healthcare billing companies.
Our coding professionals maintain expertise in:
ICD-10 diagnosis coding
CPT procedural coding
HCPCS coding standards
All coding processes align with CMS and AMA guidelines, and our professionals hold certifications from the American Academy of Professional Coders (AAPC).
Continuous training ensures our teams remain current with evolving gastroenterology coding updates and payer policies.
Best Practices for Gastroenterology Billing and Coding
MBW RCM applies structured best practices designed to improve billing accuracy and maintain compliance with gastroenterology reimbursement guidelines.
Accurate Endoscopy Documentation
Precise procedural documentation is essential for correct coding. For example, documentation must indicate whether a colonoscopy advanced beyond the splenic flexure. Without this detail, the procedure may only support coding for a sigmoidoscopy.
Correct Modifier Application
Proper use of CPT modifiers helps distinguish between multiple services performed during the same encounter and ensures accurate claim processing.
Denial Prevention Strategies
Structured workflows help identify documentation gaps and coding errors before claims are submitted, reducing the likelihood of claim denials.
Technology-Driven Billing Processes
Modern billing platforms and analytics tools support efficient claim tracking, underpayment identification, and reimbursement monitoring.
Why MBW RCM Demonstrates Expertise in Gastroenterology Billing
MBW RCM applies structured billing workflows, certified coding expertise, and technology-driven processes to manage gastroenterology billing operations.
Our revenue cycle capabilities include:
Patient demographic data entry
Insurance eligibility verification
Prior authorization management
Medical coding and claim submission
Payment posting and reconciliation
Denial analysis and resolution
Consistent accounts receivable follow-up and proactive denial prevention strategies help maintain billing accuracy and efficient reimbursement cycles.
Benefits of MBW RCM’s Gastroenterology Billing Services
Specialty expertise in gastroenterology and endoscopy billing
Certified billing and coding professionals
Compliance with CMS and AMA coding guidelines
Accurate coding for diagnostic and therapeutic GI procedures
Structured revenue cycle management workflows
Dedicated billing and coding teams
Gastroenterology billing involves a wide range of diagnostic and procedural services, from endoscopies to colonoscopies. Multiple procedures, modifiers, and biopsy coding can make billing more complex than general practice billing.
Common CPT codes include 45378–45398 for colonoscopy, 43235–43259 for EGD (esophagogastroduodenoscopy), and 91110–91112 for capsule endoscopy. Accuracy is key to avoid denials.
Frequent issues include missing prior authorizations, incorrect use of modifiers, inaccurate procedure coding, and insufficient documentation, especially for screening vs. diagnostic procedures.
MBW RCM ensures accurate coding, manages pre-authorizations, handles complex procedure combinations, and reduces denials through expert review and payer-specific billing knowledge.
Screening procedures are preventive and often fully covered by insurance. If a polyp or abnormality is found, the procedure may become diagnostic, requiring appropriate modifier and documentation for accurate billing.
Yes, but proper use of modifiers like -59 or -51 is critical. Each procedure must be justified as distinct and medically necessary, and supported with clear documentation.
Extremely important. Detailed procedure notes, patient history, and pathology findings are essential to support the codes billed and defend against audits or denials.
Yes, MBW RCM integrates with most EHR and endoscopy platforms to streamline documentation flow and reduce manual entry errors during coding and billing.
MBW RCM typically submits claims within 24–48 hours after receiving complete clinical documentation, ensuring fast reimbursement cycles for your gastroenterology practice.
Contact MBW RCM directly. Our pricing is customized based on your practice size, procedure volume, and specific needs. We offer transparent and scalable billing solutions.
Outsourcing to MBW RCM reduces administrative burden, improves claim accuracy, accelerates cash flow, and provides access to expert coders and denial prevention workflows. It enables your team to focus on patient care while we handle payer complexities, audits, and compliance monitoring. Our analytics help identify lost revenue opportunities and streamline reimbursements.
Connect with Us
Request for Information
Are you ready to streamline your revenue cycle and boost your practice's efficiency? Our specialized gastroenterology billing services help you streamline billing processes, increase ROI, and reduce administrative burden.
Benefits of Our Gastroenterology Revenue Cycle Services
-
Specializing in complex gastroenterology billing cases like colorectal screenings, we ensure precise billing for optimal reimbursement.
-
Our team's expertise in ICD-9/10, CPT, and HCPCS coding, certified by the AAPC, guarantees accurate and compliant coding for all gastroenterology services.
-
We excel in identifying and resolving underpayments, preventing significant revenue losses and ensuring the financial health of your practice.
-
Covering the entire revenue cycle, our services include patient entry, insurance verification, authorizations, and proactive denial management, streamlining your practice's operations.
-
Our analytics-driven approach focuses on reducing claim denials and increasing reimbursements, enhancing your practice's financial and operational efficiency.
-
Experience significant cost savings of 5-60% by leveraging our global delivery model to reduce operational expenses while maintaining high-quality billing and coding services. Unlock the catial you need for reinvestment into patient care and practice growth.
Resources
Explore our latest thinking